Main Content

Neurosurgery & Spine Consultants
San Antonio's Premiere Spine & Pain Treatment Clinic

Our Highly Rated Clinic is Here to Help You Live Your Best Life

Check Out Our New Bone Health Clinic!
San Antonio's Interventional Pain Management Clinic

On-Site Physical Therapy
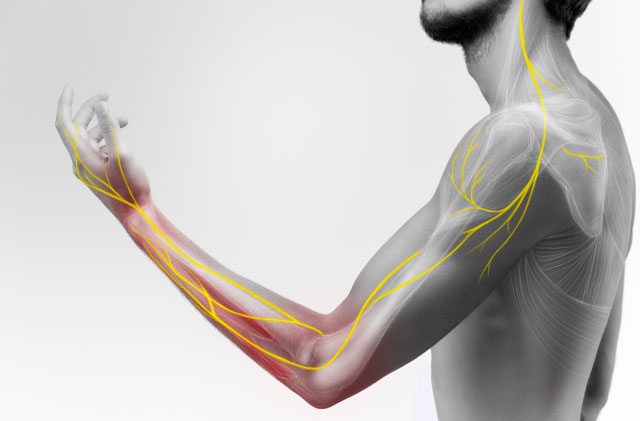
Nerve Studies (On-Site EMG/NCV)
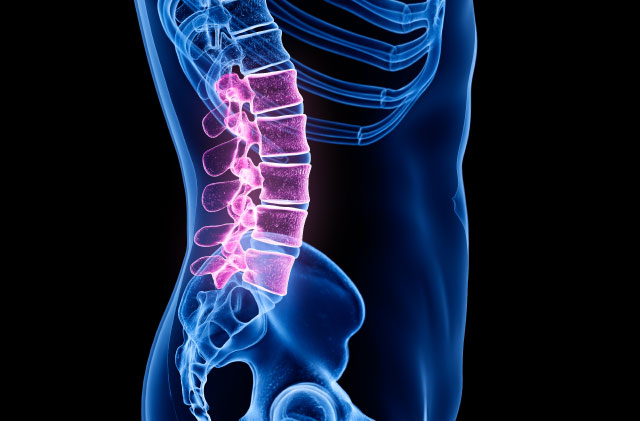
San Antonio Lumbar X-Ray Specialists
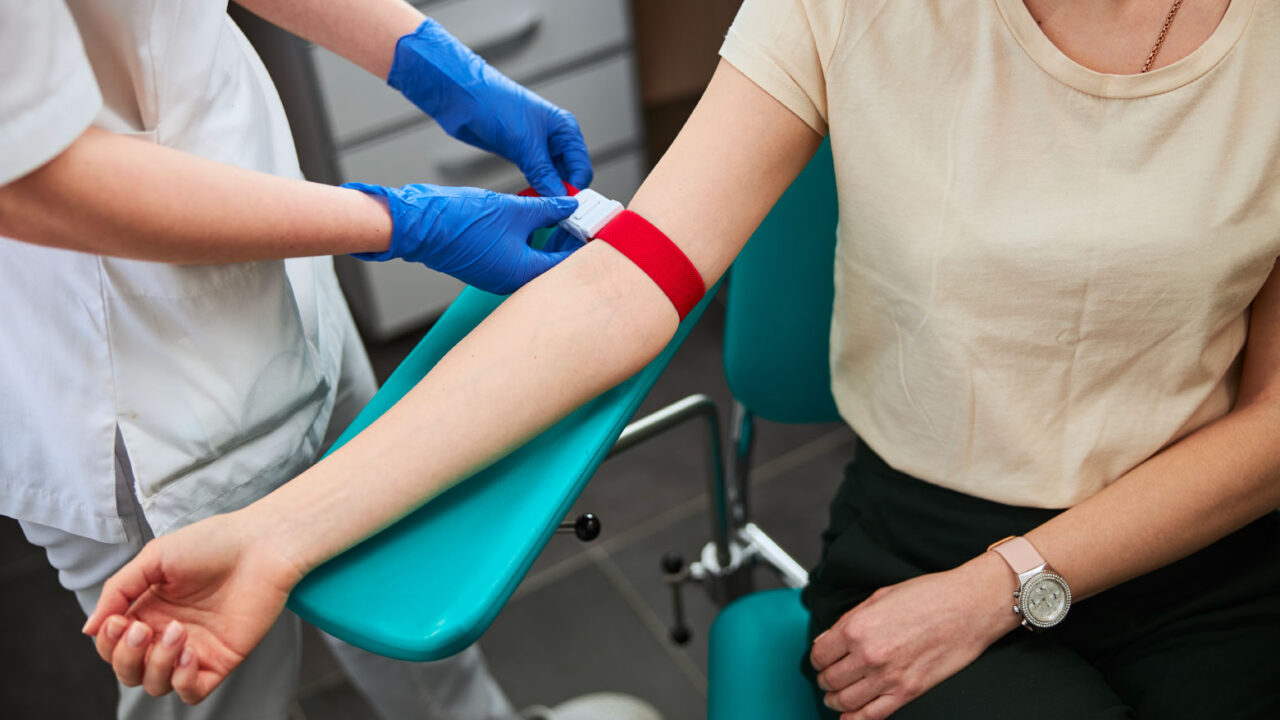
Learn More About Our On-Site Lab

Watch Alicia's Testimonial On Her Experience at NSC!

5-Star Rated Patient Experience
To provide you with compassionate care from the forefront of neurosurgery, our highly rated doctors stay active in the medical and San Antonio communities.
Minimally Invasive, Nonsurgical & Surgical Solutions for Pain
Whether or not you’ve had spine, neck, brain or peripheral nerve surgery before, our specialists will team up to provide the best solution for you.
While we’re experienced neurosurgeons and pain specialists, that doesn’t mean we only offer surgery. Think of us as brain, spine and nerve relief specialists. We work together to provide solutions for a variety of conditions, including nonsurgical treatments and minimally invasive procedures, which mean short recovery times and fast-healing incisions.
Neurosurgery & Spine Consultants emphasizes a collaborative approach to your care. We combine multiple areas of expertise under one roof to identify and relieve your pain at its source. By drawing on specialized training, decades of experience and advanced, in-house technology, we’ll design you a cautious, individualized treatment plan. Click the buttons below to read more about how we can relieve your chronic pain, spinal, cranial and nerve condition(s).
Our Care
Solutions for Your Spinal & Cranial Conditions
Disc & Vertebra Conditions
Let us help resolve your disc & vertebra conditions with our expertise.
Sciatica & Nerve Pain
Sciatica & nerve pain can be truly painful. Let us help treat the issue.
Carpal Tunnel
We're able to help provide relief from your carpal tunnel syndrome with our team of expert surgeons.
Cranial Tumors
Our neurosurgery team is dedicated to helping you overcome your cranial tumor condition.
General Inquiry
We have an outstanding record of successfully solving these complex issues with our expertise.
Patient Success Stories
“I had surgery one year ago today and I’m doing GREAT! I could not ask for a better medical team. The clinic is an awesome place too!! Any problems in the future I will be back and I have recommended to many people.” – H.H., actual patient
Meet Our Providers
4611 Centerview Dr, San Antonio, TX 78228
Reclaim what you’ve lost by ending your pain and immobility
To Request an Appointment Call 210-255-8935 or Click the Button Below









